A) Cholestyramine
B) Lactose-free diet
C) Mesalamine
D) Prednisone
E) Probiotics
G) B) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 37-year-old man comes to the office due to a week of sore throat. He also reports malaise but has had no fever, chills, nasal congestion, cough, or difficulty swallowing. Six months ago, the patient had similar symptoms and was found to have several cervical lymph nodes measuring 1.5-2 cm. Empiric antibiotic therapy was prescribed, and at follow-up 3 weeks later his sore throat had resolved and the lymph nodes were smaller. The patient has a history of hepatitis C for which he received treatment several years ago. He smokes a pack of cigarettes daily and drinks alcohol occasionally. Temperature is 37.2 C (99 F) , blood pressure is 122/68 mm Hg, and pulse is 89/min. There is pharyngeal erythema and mild tonsillar enlargement. Three nontender anterior cervical lymph nodes are palpated, measuring approximately 3 cm each. There is a 0.5-cm right posterior cervical node. The liver span is 10 cm, and the spleen cannot be palpated. Physical examination is otherwise unremarkable. Complete blood count, including peripheral blood smear, is unremarkable. Testing for HIV and rapid plasma reagin are negative. Symptomatic treatment is advised, and on follow-up 4 weeks later the patient reports his sore throat has resolved. The anterior cervical lymph nodes are decreased in size and now measure 1.5-2 cm. Which of the following is the most likely cause of this patient's lymphadenopathy?
A) Atypical mycobacterial infection
B) Epstein-Barr virus infection
C) Hepatitis C-related vasculitis
D) Lymphoid lineage neoplasm
E) Recurrent group A streptococcal infection
G) C) and D)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 28-year-old woman requests an emergency office appointment after an episode of palpitations, dizziness, chest pain, and nausea while giving a presentation at work. The patient says, "I suddenly felt dizzy and my chest was pounding. My hands and legs were tingling and I was afraid I was going to pass out." She describes several similar episodes over the past several months and worries about having another episode. She says, "I am especially afraid when it happens at work because it is so embarrassing, but it even happens when I am home doing nothing." The patient has no significant medical history. She drinks a glass of wine 3 or 4 times a week and takes no medications. Family history is significant for coronary artery disease in her father and endometrial cancer and depression in her mother. The patient appears anxious and is mildly diaphoretic. She is initially tachycardic, but repeat vital signs are within normal limits. Physical examination is unremarkable. Which of the following is the most likely diagnosis?
A) Mitral valve prolapse
B) Panic disorder
C) Paroxysmal supraventricular tachycardia
D) Performance anxiety
E) Somatic symptom disorder
G) B) and C)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 26-year-old woman, gravida 1 para 0, with a history of systemic lupus erythematosus (SLE) comes to the office for a follow-up visit. The patient is at 22 weeks gestation and feels well. She had mild nausea during the first trimester but reports no fatigue, joint or chest pain, or shortness of breath. Her SLE has been quiescent for several years and she takes hydroxychloroquine. The patient also takes a prenatal vitamin containing folic acid and iron daily. She has never smoked and does not use alcohol or illicit drugs.
Temperature is 37 C (98.6 F) , blood pressure is 116/68 mm Hg, pulse is 74/min, and respirations are 14/min. Physical examination shows no skin rash or oral ulcerations. The lungs are clear to auscultation and heart sounds are normal. Abdominal examination shows an appropriately sized gravid uterus with no tenderness. The joints are nontender and there is no edema of the extremities.
Laboratory results are as follows:
 Prepregnancy hemoglobin was 13.2 g/dL and at 8 weeks gestation was 12 g/dL.
Which of the following is the most appropriate next step in management of this patient?
Prepregnancy hemoglobin was 13.2 g/dL and at 8 weeks gestation was 12 g/dL.
Which of the following is the most appropriate next step in management of this patient?
A) Close observation only
B) Direct antiglobulin (Coombs) test
C) Increase iron supplementation
D) Lactate dehydrogenase and haptoglobin levels
E) Serum vitamin B12 and folate levels
G) C) and D)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 56-year-old woman comes to the physician for evaluation of a right adrenal mass found 2 weeks ago on an abdominal CT scan performed for renal colic. The lesion is 2 cm in diameter, round, and has low x-ray attenuation (8 Hounsfield units) on non-contrast slices. Her other medical problems include hypertension treated with amlodipine. Family history is unremarkable.
Her blood pressure is 144/96 mm Hg, pulse is 66/min, and BMI is 26 kg/m2. The remainder of the examination is within normal limits.
Laboratory results are as follows:
 Which of the following is the most appropriate next step in managing this patient?
Which of the following is the most appropriate next step in managing this patient?
A) Add hydrochlorothiazide and follow-up in 4 weeks
B) Aldosterone to renin ratio
C) Fine needle aspiration of the mass
D) Repeat CT scan of the abdomen in 6 months
E) Unilateral laparoscopic right adrenalectomy
G) A) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
Cardiovascular disease is the leading cause of morbidity and mortality in women in developed countries. Based on current evidence, which of the following is true for women as compared with men?
A) Women are less likely to receive aggressive treatment for chest pain.
B) Women are more likely to be referred for cardiac catheterization for abnormal stress testing.
C) Women are more likely to get false-positive results on stress imaging studies.
D) Women are more likely to present with typical angina.
E) Women have a lower burden of risk factors during presentation for coronary heart disease.
G) A) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 56-year-old man comes to the physician because of an intermittent, non-pruritic skin rash that appeared approximately one year ago. The rash starts as skin irritation followed by blistering and then crusting that is sometimes very painful. The rash affects the back of his hands and sometimes his neck. He initially thought the irritation was caused by his soap, but switching to a different brand did not help. He feels he is in good health otherwise and does not see doctors. He was told that he has "borderline diabetes" and high blood pressure several years ago. He is a former intravenous drug abuser. He smokes one pack of cigarettes per day and drinks beer over the weekend. His blood pressure is 152/77 mm Hg and pulse is 82/min. His BMI is 32 kg/m2. The oral mucosa is moist without any lesions. There is no lymph node enlargement. Lungs are clear to auscultation and there are no heart murmurs. Abdomen is non-tender. Inspection of the skin reveals areas of erosion, crusting, skin hyperpigmentation, and fine scarring affecting the dorsum of both hands, ears, extensor surfaces of the arms, and the back of the neck. Which of the following is most likely related to this patient's condition?
A) Chronic viral hepatitis
B) Fat malabsorption
C) Insulin resistance
D) Occult lung malignancy
E) Parasitic infection
G) A) and B)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 33-year-old woman comes to the office due to a 2-day history of severe left knee pain and swelling. She has had no trauma, pain in other joints, fever, chills, or rash. The patient has a history of parathyroid adenoma with primary hyperparathyroidism and underwent parathyroidectomy a week ago. Her other medical problems include moderate persistent asthma, irritable bowel syndrome, and gastroesophageal reflux disease. The patient does not use tobacco, alcohol, or illicit drugs. She is married and her only medication is an oral contraceptive.
Temperature is 36.7 C (98 F) , blood pressure is 110/56 mm Hg, pulse is 67/min, and respirations are 14/min. BMI is 28 kg/m2. Physical examination shows a moderate left knee effusion with warmth, erythema, and tenderness. Range of motion of the knee is decreased due to pain.
Laboratory results are as follows:
 Analysis of synovial fluid from the knee joint shows a leukocyte count of 20,400/mm3 with 80% neutrophils.
Which of the following is the most likely cause of this patient's knee pain?
Analysis of synovial fluid from the knee joint shows a leukocyte count of 20,400/mm3 with 80% neutrophils.
Which of the following is the most likely cause of this patient's knee pain?
A) Acute gouty arthritis
B) Erosive osteoarthritis
C) Osteitis fibrosa cystica
D) Pseudogout
E) Septic arthritis
G) B) and C)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 58-year-old woman comes to the walk-in clinic with 2 days of right thigh pain. She has hypertension and her medications include chlorthalidone and lisinopril. She also has been told that she is pre-diabetic. Her BMI is 32 kg/m2. The patient's blood pressure is 152/80 mm Hg and pulse is 87/min. A tender, nodular cord is palpated along the inner upper-right thigh. There are no skin changes. There is no ankle edema. Her previous laboratory results were notable for creatinine of 1.3 mg/dL and HbA1c of 6.7%. Which of the following is the best next step in managing this patient?
A) Advise cold compresses and low-dose aspirin
B) Order hypercoagulability workup
C) Order venous duplex scan of the legs
D) Prescribe naproxen and follow up in 7-10 days
E) Schedule pelvic ultrasound
G) C) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 42-year-old woman comes to the physician with 6 months of progressively worsening exertional dyspnea. She is unable to climb two flights of stairs without becoming short of breath. She also complains of dry cough, weight loss, and fatigue. She describes finger tingling and numbness when exposed to colder temperatures. Her past medical history is significant for acid reflux disease and diabetes mellitus. Her medications include metformin and omeprazole. She does not smoke cigarettes.
Her blood pressure is 155/80 mm Hg and her pulse is 86/min. Oxygen saturation is 94% on room air. Small ulcers are seen at the fingertips bilaterally. Jugular venous pressure is estimated at 6 mm H2O. There are no heart murmurs. Inspiratory fine crackles are heard on auscultation at lung bases. There is no organomegaly.
Laboratory results are as follows:
 Chest x-ray shows bilateral reticular opacities.
Which of the following antibodies is most likely to be positive in this patient?
Chest x-ray shows bilateral reticular opacities.
Which of the following antibodies is most likely to be positive in this patient?
A) Anticitrullinated peptide antibodies
B) Anti-DNA topoisomerase I antibodies
C) Antimitochondrial antibodies
D) Antineutrophil cytoplasmic antibodies
E) Antisynthetase antibodies
G) A) and B)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 48-year-old woman comes to the emergency department due to "fluttering" in her chest and 10/10 nonradiating chest pain. She feels as if "someone is sitting on my chest." The patient has had similar episodes during the past 6 months that occur at rest and with exertion. In addition to the chest pain, she experiences dyspnea, dizziness, paresthesias, and abdominal cramping. She has also noticed that she fears and avoids being in public places such as crowded shopping malls and restaurants. The patient now insists that her husband drive her to work due to fear of having an attack while driving alone. Over the past month, she has left work on multiple occasions due to the episodes and worries that she will have to stop working or be fired for repeated absences. The patient is an administrative assistant with an approximately 20-year smoking history. She does not use other substances and her medical history is insignificant. She is postmenopausal. Her father and paternal uncle suffered myocardial infarctions in their 50s. Temperature is 37.2 C (99 F) , blood pressure is 130/80 mm Hg, pulse is 94/min, and respirations are 18/min. The patient is a well-developed woman who appears her stated age. She is anxious and diaphoretic. Physical examination is otherwise normal. ECG shows no evidence of an ischemic event. Laboratory studies, including complete blood count, chemistries, liver function, and urinalysis, are within normal limits. The patient has negative serial troponin and CK-MB levels. Which of the following is the most appropriate pharmacotherapy for this patient's symptoms?
A) Aripiprazole and alprazolam
B) Bupropion and paroxetine
C) Clonazepam and fluoxetine
D) Risperidone and propranolol
E) Sertraline and buspirone
G) B) and D)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 35-year-old woman comes to the office due to a 6-month history of diarrhea. She has had several loose stools per day without visible blood or mucus. The patient has also noticed bloating and abdominal discomfort following meals. She eats a varied diet and cannot identify any particular foods associated with her symptoms. The patient is unsure if she has lost weight but says that her friends have remarked that she "doesn't look healthy." The patient's medical history includes iron-deficiency anemia and menorrhagia. Her only medication is an oral iron supplement and she has no known drug allergies. Family history is remarkable for hypothyroidism in her mother. The patient has had no recent travel and works from home. Temperature is 36.4 C (97.5 F) , blood pressure is 115/63 mm Hg, pulse is 70/min, and respirations are 14/min. Sclera are anicteric and mucous membranes are moist. Auscultation of the heart and lungs is normal. The abdomen is soft and nontender. Bowel sounds are hyperactive. Rectal examination is normal, and fecal occult blood testing is negative. No skin rashes are present. The remainder of the examination is unremarkable. Laboratory results show a hemoglobin of 9.6 mg/dL with mean corpuscular volume of 71 µm3. Anti-tissue transglutaminase antibody is positive. Which of the following is the most appropriate next step in management of this patient?
A) Antigliadin antibody testing
B) Endoscopy with duodenal biopsy
C) Gluten-free diet with close follow-up for symptom resolution
D) Human leukocyte antigen testing
E) Total IgA level testing
G) A) and D)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 26-year-old woman comes to the office due to persistent fatigue and inability to lose weight. She has also experienced hair loss and dry skin. The patient was diagnosed with primary hypothyroidism 2 years ago and was started on levothyroxine therapy, which she takes on an empty stomach every morning. She exercises 5 times per week, follows very strict caloric restrictions, and has eliminated gluten-containing foods from her diet. Medical history is unremarkable, and the patient has never been pregnant. In addition to levothyroxine, she also takes a cyclic estrogen-progestin oral contraceptive. The patient is sexually active with one partner and does not use tobacco, alcohol, or illicit drugs.
Blood pressure is 124/80 mm Hg and pulse is 70/min. BMI is 26 kg/m2. The thyroid gland is diffusely enlarged, firm, and nontender, and the remainder of the physical examination is normal.
Laboratory results are as follows:
 Which of the following is the most appropriate next step in management of this patient's condition?
Which of the following is the most appropriate next step in management of this patient's condition?
A) Add liothyronine (T3) to current therapy
B) Continue current therapy and evaluate other etiologies
C) Discontinue oral contraceptives
D) Increase levothyroxine dose
E) Initiate selenium therapy
G) B) and C)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 42-year-old man comes to the office because of heartburn. He has had these symptoms for the past 3 months. He states that symptoms occur almost daily and he has experienced nocturnal awakening because of regurgitation at least twice weekly. This has caused him daytime fatigue and poor concentration at work. He also complains of dry cough and wheezing. He denies any difficulty swallowing, nausea, vomiting, or weight loss. He has tried over-the-counter antacids with no significant relief.
His other medical problems include hypertension and mild intermittent asthma. He does not use tobacco, alcohol, or drugs. His father suffered from colon cancer at the age of 68 and his mother died of breast cancer at the age of 72. His medications include hydrochlorothiazide and lisinopril. He uses albuterol as needed for shortness of breath. He has no known drug allergies.
His blood pressure is 138/89 mm Hg and pulse is 87 /min. His BMI is 30 kg/m2. Physical examination is unremarkable.
Laboratory results are as follows:
 Which of the following is the most appropriate next step in management?
Which of the following is the most appropriate next step in management?
A) Barium swallow
B) Daily metoclopramide
C) Daily proton pump inhibitor
D) Pulmonary function testing
E) Upper GI endoscopy
G) A) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 45-year-old man comes to the physician due to 2 weeks of muscle stiffness and imbalance. He has no fever, headache, joint pain, or muscle soreness. The patient has a history of bipolar disorder and suicidal ideations. He was started on risperidone for a manic episode 2 months ago. He does not use alcohol or tobacco. His blood pressure is 130/80 mm Hg and pulse is 68/min. On examination, there is a low-amplitude resting tremor of both hands. Finger tapping is slow and irregular on both sides. Which of the following is the most appropriate next step in management of this patient?
A) Change risperidone to quetiapine
B) Obtain brain MRI
C) Obtain thyroid function tests
D) Start benztropine
E) Start pramipexole
G) B) and D)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 22-year-old woman comes to the physician with several depigmented skin lesions on her hands and feet. She has no other physical complaints. Her past medical problems include migraine headaches, for which she takes naproxen as needed. She is married and has an 8-month-old child. Vital signs are within normal limits. Skin examination findings are shown below. Which of the following is the most appropriate next step in management of this patient?
A) Antimitochondrial antibodies
B) Antinuclear antibodies
C) Intralesional corticosteroid injections
D) Skin biopsy
E) Thyroid-stimulating hormone
G) D) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 65-year-old man is evaluated for a 6-month history of unsteady gait. His balance has become so poor that he requires the use of a cane. The patient also has paresthesias in his hands and feet, which started a year ago. He has a medical history of lumbar spinal stenosis, hypertension, and hyperlipidemia. The patient has a 30-pack-year smoking history and does not use alcohol or illicit drugs.
Blood pressure is 143/90 mm Hg and heart rate is 82/min. Neurologic examination reveals a distal greater than proximal reduction in pain and temperature sensation, vibration, and proprioception in the lower and upper extremities. Muscle bulk, tone, and strength are normal. Ankle reflexes are absent with downgoing plantar responses. His gait is high-stepping, and Romberg sign is positive. Laboratory results are as follows:
 Which of the following tests is most likely to establish the diagnosis in this patient?
Which of the following tests is most likely to establish the diagnosis in this patient?
A) Lumbar puncture
B) Lyme disease serology
C) MRI of the brain and spine
D) Serum immunofixation electrophoresis
E) Urine and blood for porphyrins
G) A) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 54-year-old man comes to the office due to seeing double while watching TV at night. The sensation resolves when he closes either eye. The patient gets a mild headache when he experiences double vision but has no associated nausea, vomiting, photophobia, or phonophobia. According to his wife, his voice gets a little "nasal" in the evening. He has no other medical problems and does not use tobacco, alcohol, or illicit drugs.
The patient's vital signs are normal. His eyes are shown in the image below. Eye movements are full, and pupils are equal and equally reactive to light with a brisk response. Funduscopic examination is normal. There is no extremity weakness or sensory loss. He is stable in the Romberg position. The remainder of the physical examination is normal.
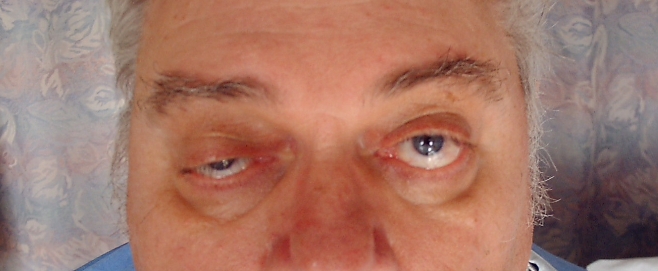 Which of the following is the best next step in management of this patient?
Which of the following is the best next step in management of this patient?
A) Autoantibody testing
B) CT scan of the chest
C) Edrophonium test
D) Prednisone therapy
E) Pyridostigmine therapy
G) B) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 35-year-old man comes to the office for increasing anxiety associated with public speaking. The patient previously worked in product development but was recently promoted to a leadership sales position that requires leading daily team meetings and frequent public speaking. When speaking before a group of people, the patient becomes extremely anxious; his face turns bright red; he starts to sweat profusely; and he feels that his heart is racing. He also becomes acutely aware that other people notice his anxiety and judge him negatively. The patient reports that he has been uncomfortable in large groups and while meeting new people since he was a teenager. His new job has been very stressful as he can no longer avoid these situations. He recognizes that his anxiety and fear of public speaking are excessive. The patient has no depression and is otherwise healthy. Blood pressure is 118/68 mm Hg and pulse rate is 86/min. BMI is 23 kg/m2. The remainder of the physical examination is unremarkable. Which of the following is the most appropriate pharmacologic treatment in management of this patient?
A) Alprazolam
B) Buspirone
C) Clonazepam
D) Propranolol
E) Sertraline
G) A) and E)
Correct Answer

verified
Correct Answer
verified
Multiple Choice
A 72-year-old man comes to the physician complaining of difficulty swallowing for the last 6 months. He reports that food gets stuck in the back of his throat. His wife notes that he often sounds "gurgly" and has bad breath throughout the day. He has lost 4.53 kg (10 lb) over the last 3 months since being discharged from the hospital with pneumonia. The patient's other medical problems include hypertension, gout, and gastroesophageal reflux disease. He is a lifetime nonsmoker and does not drink alcohol.
His blood pressure is 146/78 mm Hg, pulse is 84/min, and respirations are 14/min. Examination shows moist mucous membranes. There are no oral lesions or cervical lymphadenopathy. Scattered wheezes are heard at the right lung base. The abdomen is soft and nontender.
Laboratory results are as follows:
 Which of the following is the most appropriate next step in management?
Which of the following is the most appropriate next step in management?
A) Barium swallow
B) Computed tomography of neck and chest
C) Esophageal manometry
D) Esophagogastroduodenoscopy
E) Impedance testing
G) A) and E)
Correct Answer

verified
Correct Answer
verified
Showing 361 - 380 of 900
Related Exams